Twelfth nerve palsy in Sjogren’s syndrome
Youssef Kort, Nahed Kessentini, Naziha Khammassi & Heykel Abdelhedi
Cite this article as: BJMP 2016;9(4):a933
|
|
Abstract We report the case of a 62-year-old patient suffering from a sicca syndrome for 6 years. The diagnosis of a primary Sjögren’s syndrome was made according to the European American study group criteria. Her mouth examination showed a fissured, smooth and left deviated tongue without evidence of atrophy or fasciculation. Neurological examination confirmed the deficit of the right XII cranial nerve and excluded other cranial nerves involvements. Cranial nerve palsy (especially optic neuritis and trigeminal palsy) is a possible neurological manifestation of Sjögren’s syndrome. However, hypoglossal involvement is very uncommon and only two cases have been described in English literature. Keywords: Cranial nerve palsy, sjogren syndrome |
Background
Sjögren’s syndrome (SS) is an autoimmune exocrinopathy characterised by a lymphoplasmacytic infiltration of the exocrine glands. Both xerophthalmia and xerostomia are the most common manifestations of the disease. However serious organ damage such as, pulmonary and neurological involvement, can occur. The prevalence of neurological manifestations of SS varies between 0% and 70% (average 20%), which is largely dominated by peripheral neuropathies¹. The cranial nerve involvement, especially when it is isolated, represents a rare facet of the peripheral neuropathy.
Observation
We report the case of a 62-year-old patient with no medical history, referred to the internal medicine department with a 6 years history of dry mouth and xerophthalmia. No other complaints were reported.
The mouth examination showed a fissured, smooth and left deviated tongue without evidence of atrophy or fasciculation (figure 1). The rest of the oropharyngeal examination was unremarkable with no angina or cervical lymphadenopathy. Neurological examination confirmed a deficit of the right XII cranial nerve and excluded other cranial nerve involvements, sensibility or motility deficit. A specialised ophthalmologic examination was performed and showed a bilateral superficial punctuate keratitis.
The search for antinuclear antibodies by indirect immunofluorescence was positive at the titre of 1/1280 (speckled) corresponding to Anti-SSA and Anti-SSB antibodies. Cryoglobulinemia search was negative.
The rest of the laboratory investigations (blood cell count, liver and renal function tests, thyroid balance and inflammation markers) were normal.
A labial salivary gland biopsy was performed and its histological examination showed a lymphoid cell cluster of more than 50 cells/ 4 mm² corresponding to a focus score 1.
Brain MRI was normal - no damage in the brain stem was seen. Electromyography was normal.
The diagnosis of SS was made according to the presence of five out of six criteria according to the European American study group. The diagnosis of primary SS was retained due to the lack of clinical or biological argues for an associated autoimmune disease. A symptomatic treatment of Sicca syndrome was prescribed but no specific therapy has been initiated for the hypoglossal nerve attempt because of its asymptomatic nature.
Discussion
In the case of our patient, the tongue deviation was discovered at physical examination and was totally asymptomatic. In other cases, the twelfth nerve palsy could be responsible for swallowing difficulties, and in advanced stages for a lingual or hemi lingual amyotrophy. The spectrum of its aetiologies is numerous. In a large case series of 100 patients, malignant tumors (about half of cases), neurological causes (16 %) and post-traumatic palsy (12% of cases) were the three most popular aetiologies². Other conditions could be associated with twelfth nerve palsy, such as, infections², vascular injury³ and non-invasive oxygen therapy⁴. Paroxysmal idiopathic hypoglossal nerve palsy has also been described⁵. Our patient had Sicca syndrome which was related to SS according to 5 criteria of the European American study group: it was a subjective sensation of dry mouth and dry eyes associated to a bilateral punctuated keratitis, a focus score > 1 at the histological examination of the salivary gland biopsy and positive anti-SSA and anti-SSB⁶.
SS is an autoimmune disease that often presents as dry eyes and dry mouth due to lacrimal and salivary gland involvement. It can be primitive or associated to other autoimmune diseases such as, Hashimoto’s Thyroiditis, Rheumatoid Arthritis or Systemic Lupus Erythematosus. Wide varieties of neurological complications are characteristic features of SS which occurs most frequently in the primary form. Peripheral neuropathy is the most frequent neurological manifestation. Its most common presentation is a symmetrical sensorimotor or pure sensory neuropathy of hands and feet. Sensitive neuropathy, small fiber neuropathy, multiple mononeuropathy and polyradiculoneuropathy have also been described¹. Cranial nerve involvement is rare. In a review of the literature, Colaci M found 267 patients suffering from SS with different types of cranial neuritis during their clinical history. The discovery of cranial neuritis was contemporary to SS diagnosis in 40% of the patients, as in the case of our patient.
Optic neuritis and trigeminal nerve injury were the most frequent attempts and represent respectively 46.4% and 38% of all cranial nerve palsies. All cranial nerves palsies have been described except the eleventh⁷. Involvement of the twelfth cranial nerve is very rare and only two cases have been described⁸′ ⁹. In these two cases, it was associated with an involvement of other cranial nerves (table 1). To the best of our knowledge, this is the first report of an isolated and permanent involvement of the twelfth cranial nerve in a patient with primary SS. Many mechanisms were proposed to explain the cranial nerve involvement in SS. Clinicopathological observations of Mori K⁸ suggest that an isolated trigeminal nerve attempt could be explained by an immune-mediated neuron death in the sensory gasser ganglion. Whereas, other cranial nerve involvements which are frequently associated together could be explained by a multiple mononeuropathy resulting from a vasculitis⁸.
Further clinical observations will be necessary to determine the exact mechanisms of such neurological involvement.
Table 1: Review of the literature regarding SS patients with hypoglossal nerve injury
| Number of patients | Age | Nerves
involved |
Treatment | Evolution | |
| Mori/2005 [8] | 1 | No data | V, VII, IX, X, XII | No data | Paroxysmal |
| Ashraf/2009 [9] | 1 | 47 | V–IX–XII | No data | Paroxysmal |
| Our patient | 1 | 62 | XII | None | Permanent |
Figure 1: Smooth and left deviated tongue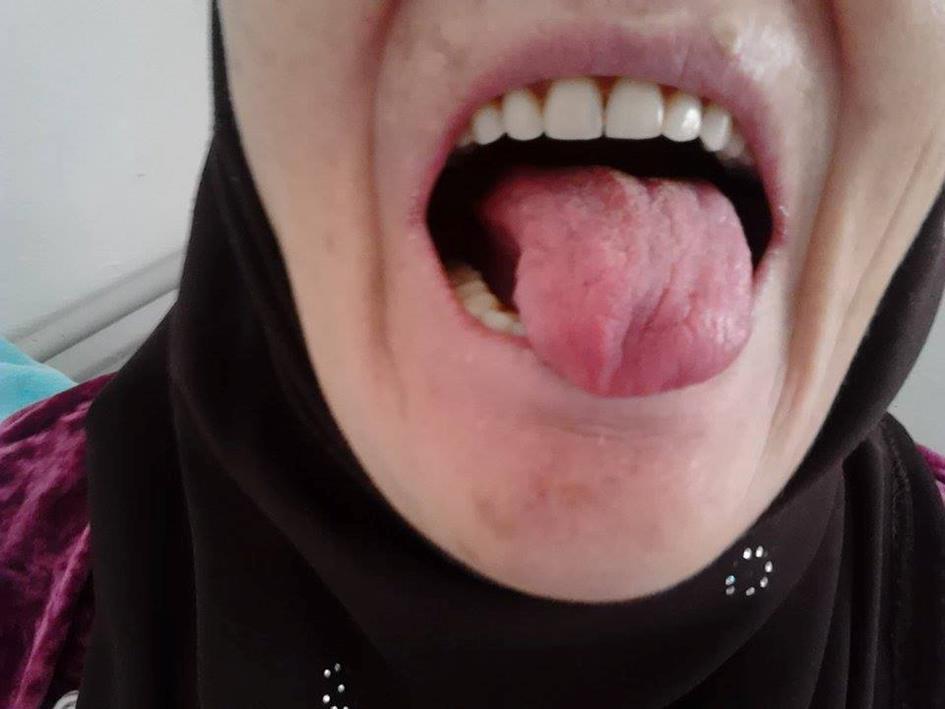
Conclusion
In front of cranial nerves neuritis, we should actively search for sicca syndrome, sometimes not spontaneously reported by patients. Examination of the mouth can be instructive and should not be omitted in the diagnosis and monitoring of Sjögren’s syndrome.
|
Competing Interests None declared Author Details YOUSSEF KORT, Doctor, Razi Hospital, Tunisia. NAHED KESSENTINI, Doctor, Razi Hospital, Tunisia. NAZIHA KHAMMASSI, Doctor, Razi Hospital, Tunisia. HEYKEL ABDELHEDI, Doctor, Razi Hospital, Tunisia. CORRESPONDENCE: YOUSSEF KORT; Razi hospital, 2010, Tunisia Email: y_kort@yahoo.fr |
References
- Carvajal Alegria G, Guellec D, Devauchelle-Pensec V, Saraux A. Is there specific neurological disorders of primary Sjögren's? Joint Bone Spine. 2015 Mar;82(2):86-9.
- Keane JR. Twelfth-nerve palsy. Analysis of 100 cases. Arch Neurol. 1996 Jun;53(6):561-6.
- Mahadevappa K, Chacko T, Nair AK. Unilateral Hypoglossal Nerve Palsy Due to Vertebral Artery. Clin Med Res. 2012 Aug;10(3):127-30.
- Weissman O, Weissman O, Farber N et al. Hypoglossal nerve paralysis in a burn patient following mechanical ventilation. Ann Burns Fire Disasters. 2013 Jun 30;26(2):86-9.
- Ibarra V, Jaureguiberry A, Moretta G, Lazzarini G, Ceruzzi R, Reich E. Idiopathic and unilateral hypoglossal nerve palsy. Medicina . 2015;75(3):173-4.
- Vitali C, Bombardieri S, Jonsson R et al. Classification criteria for Sjögren's syndrome: a revised version of the European criteria proposed by the American-European Consensus Group. Annals Rheumatology Disease. 2002;61(6): 554–58.
- Colaci M, Cassone G, Manfredi A, Sebastiani M, Giuggioli D, Ferri C. Neurologic Complications Associated with Sjögren’s Disease: Case Reports and Modern Pathogenic Dilemma. Hindawi Publishing Corporation, Case Reports in Neurological Medicine. Case Rep Neurol Med.; 2014: 590292.
- Mori K, Iijima M, Koike H et Al. The wide spectrum of clinical manifestations in Sjogren's syndrome-associated neuropathy. Brain. 2005; 128:2518-34.
- Ashraf VV, Bhasi R, Kumar RP, Girija AS. Primary Sjogren’s syndrome manifesting as multiple cranial neuropathies: MRI findings. Annals of Indian Academy of Neurology.2009; 12(2):124–126.

The above article is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License.




