Photo Quiz: Localized, reticulated erythema
Andrew A Lawson & Thomas C Michels
Cite this article as: BJMP 2017;10(1):a1004
|
|
Abstract A 70-year-old man presented in the winter with a four-week history of redness of the left anterolateral leg. On exam, the patient has an 8 cm, irregular patch of reticulated erythema with both hyperpigmentation and scaling. This manuscript contains the history and physical exam, a photo of the lesion, a differential diagnosis, and a discussion of management. Keywords: Erythema ab igne, reticulated erythema, livedo reticularis, livedo racemosa, first-degree burnAbbreviations: EAI - Erythema ab igne |
A 70-year-old man presented in the winter with a four-week history of redness of the left anterolateral leg. He first noticed a slight “tenderness” in the area when showering; the discomfort lasted only a few days. Over the next week, he noticed redness developing. It is now painless and not pruritic, warm, or peeling. He has not applied any topical lotions or creams. He has not had an exposure to new soaps or detergents. He feels well, without fever or weight loss. He has a diagnosis of hypertension and lumbar radiculopathy with an L5 discectomy and resultant leg numbness. He is retired and does not smoke or drink alcohol; his hobby is woodworking in his garage.
Physical examination reveals normal vital signs. On his left anterolateral leg, he has an 8 cm, irregular patch of reticulated erythema with both hyperpigmentation and scaling. The lesion is non-palpable. He has decreased sensation in an L5 distribution on that leg, which was unchanged from prior examinations. These skin findings are shown in Figure 1.
Figure 1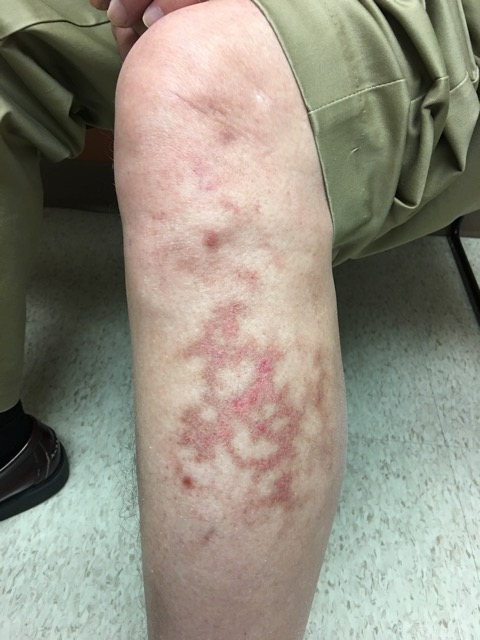
Question: Based on history and physical examination, which of the following is the most likely diagnosis?
- Livedo reticularis
- Erythema ab igne
- Livedo racemosa
- First-degree burn
Discussion
The answer is erythema ab igne (EAI; literally “redness from fire,”) which results from chronic exposure to moderate-intensity heat. EAI presents as a reticulated erythematous patch over the area of exposed skin. Possible secondary changes include epidermal atrophy and scaling.1,2 With repeated exposure, brown hyperpigmentation may develop.1 Most patients are asymptomatic, although some note a mild burning sensation. A history of repeated exposure to heat is key to the diagnosis. While cases were historically noted on skin exposed to fire, such as the arms of bakers and coal shovellers, EAI can result from our many, modern heat-sources, such as laptop computers, car seat heaters, heating pads, and, in this case, the portable space heater under the patient’s woodworking bench.2-4 With removal of the heat source, hyperpigmentation typically regresses but may take years.1,3 The diagnosis is clinical. A biopsy is not required to make the diagnosis, but is indicated if malignant transformation is suspected. EAI can increase risk of squamous cell carcinoma, Merkel cell carcinoma, and cutaneous marginal zone lymphoma.1,5 Treatment is typically not necessary; topical steroids or retinoids and laser have had variable success.1,3,4 If pre-malignant changes are detected, topical 5-flourouracil is recommended.1,4
See Table 1 for a summary of the key characteristics and distinguishing features of each diagnosis in this selected differential.
Table 1. Selected Differential Diagnosis of Reticulated Skin Lesions in Adults
| Condition | Characteristics |
| Livedo reticularis | Violaceous mottled or reticulated patches; painless; typically temperature sensitive; may be physiologic or secondary to systemic disease; no hyperpigmentation. |
| Erythema ab igne | Erythematous reticulated patch, with possible secondary changes including epidermal atrophy and scaling; chronic exposure may lead to hyperpigmentation; painless or associated with a mild burning sensation; history of heat exposure. |
| Livedo racemosa | Violaceous reticulated patch with larger branching pattern than livedo reticularis, often with asymmetric or “broken” net appearance; typically involves the trunk and proximal limbs; generally secondary to chronic disease; frequently painful; no hyperpigmentation. |
| First-degree burn | Erythematous, dry, painful lesion which includes the entire area of skin that contacted the high-intensity heat source; not reticulated; no hyperpigmentation. |
Livedo reticularis is typically more violaceous in appearance, with net-like, mottled discolouration of the skin due to deoxygenation and dilation of the venous plexus. Primary, physiologic livedo reticularis is often brought on by cold and alleviated by warming. It usually involves a larger area, such as the bilateral thighs, rather than a confined area of skin.1,2
Livedo racemosa is a persistent variant of livedo reticularis with a characteristic, large, broken, branching pattern, often on the trunk and proximal limbs. It is generally secondary to a systemic disease, such as antiphospholipid antibody syndrome or Sneddon syndrome.6
First-degree burns are erythematous, dry, and painful. Instead of a reticulated pattern, as shown here, the erythema of first degree burns covers the entire area of skin that contacted the high-intensity heat source.
|
Acknowledgements None Competing Interests None declared Author Details ANDREW LAWSON, BS, 8253 Bagley Ave N., Seattle, WA 98103, USA. THOMAS MICHELS, MD, MPH, 1037 NE 65th St #80631, Seattle, WA 98115, USA. CORRESPONDENCE: ANDREW LAWSON, 8253 Bagley Ave N., Seattle, WA 98103, USA Email: aalawson@uw.edu |
References
- Miller K, Hunt R, Chu J, et al. Erythema ab igne. Dermatology Online Journal. 2011;17(10):28.
- Riahi RR, Cohen PR. What Caused This Hyperpigmented Reticulated Rash On This Man’s Back? The Dermatologist. 2013;21(1). http://www.the-dermatologist.com/content/what-caused-hyperpigmented-reticulated-rash-man%E2%80%99s-back
- Salgado F, Handler MZ, Schwartz RA. Erythema ab igne: new technology rebounding upon its users? Int J Dermatol. 2017. doi: 10.1111/ijd.13609. [Epub ahead of print]
- Beleznay K, Humphrey S, Au S. Erythema ab igne. CMAJ. 2010;182(5):E228.
- Sigmon JR, Cantrell J, Teague D, et al. Poorly differentiated carcinoma arising in the setting of erythema ab igne. Am J Dermatopathol. 2013;35(6):676-8.
- Uthman IW, Khamashta MA. Livedo racemosa: a striking dermatological sign for the antiphospholipid syndrome. J Rheumatol. 2006;33:2379-2382.

The above article is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License.




