A case of bilateral swelling of the hands in an elderly gentleman
Vijay Joshi, Anna Green and Jane Griffin
Cite this article as: BJMP 2009:2(1) 44-45
|
Abstract
Remitting seronegative symmetrical synovitis with pitting edema (RS3PE) is a rare clinical syndrome, commonly seen in elderly patients who present with dorsal pitting edema of the hands and has a dramatic response to steroids, suggesting a benign nature. Sometimes it is associated with other rheumatologic conditions and potential underlying malignancy should be ruled out, especially when there is a poor response to steroids.
Key words ;
Symmetrical synovitis, seronegative arthritis, PMR, paraneoplastic arthritis
Elderly patients presenting with musculoskeletal symptoms such as painful, swollen or stiff jointsare challenging to physicians. The common conditions encountered are osteoarthritis, crystal arthropathies, spondyloarthropathies and rarely seropositive arthritis. RS3PE highlights a different inflammatory disease involving the tenosynovium of the tendons of the hands with a characteristic presentation. This case details such a presentation and aims to raise awareness amongst general physicians.
Case report:
An 83 year old man, with a history of chronic leg ulcers and poor mobility presented following a fall at home. On admission he also complained of a six to eight week history of bilateral hand swelling. This was of sudden onset, initially on the right hand and gradually progressed until the time of admission when it became prominent over the dorsum of both hands. Both hands were initially tender, but painfree at rest, and restricted in movement due to the swelling. Lately he had also noticed mild inactivity stiffness in his knees and shoulders, He had no previous musculoskeletal history, no skin rash or trauma to his hands.
Inspection of his hands revealed bilateral, symmetrical swelling, involving all the fingers and more pronounced on the dorsum. On palpation there was pitting oedema over the dorsum without signs of synovitis or joint deformity.(Figure 1 and 2).
On movement, finger flexion and opposition were limited, with reduced grip strength.
There was no girdle muscle weakness or pain. There was pitting oedema of both feet, with compression bandaging to the upper calf. This was chronic, and was likely to be secondary to peripheral vascular insufficiency.
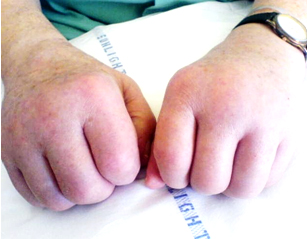
Fig 1:Swollen hands

Fig 2: Dorsal pitting edema
Blood tests during this admission showed normocytic anaemia with low vitamin B12 levels but normal ferritin. Erythrocyte sedimentation rate (ESR) was raised at 100mm/hour and initial C-reactive protein (CRP) at 55 mg/l. Anti nuclear antibody (ANA) and rheumatoid factor were negative. X-rays of the hands revealed mild osteoarthrosis without any evidence of bony erosions. Computerised tomography (CT) of the chest and abdomen did not show any evidence of malignancy.
In view of the clinical presentation and seronegativity, a diagnosis of peritendinous rheumatoid arthritis was considered. He was commenced on low dose oral steroids following initial parenteral corticosteroid. Subsequent to the initiation of steroids, there was dramatic resolution of the swelling of the hands, within a week (Figure 3),
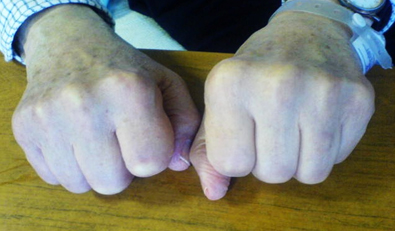
Fig 3: Response to steroids
Case discussion
Remitting seronegative symmetrical synovitis with pitting edema (RS3PE) syndrome was first described by McCarty et al in 1985 1 . It is also termed as peritendinous rheumatoid arthritis in Europe.
It predominantly affects elderly males and although not exceptionally rare, there is no clear documentation of the incidence of this condition (2).
The syndrome is a subset of symmetrical polyarthritis characterised by
-
Bilateral pitting oedema of both hands
-
Sudden onset of polyarthritis (A few cases report patients being able to state the time to the hour at which this occurred.1)
-
Age >50 years
-
Absence of rheumatoid factor (seronegativity).
Other features include symmetrical distal synovitis and tenosynovitis affecting the synovial sheaths of the flexor and extensor tendons of the hands and/or feet without evidence of joint erosions 2. It responds dramatically to corticosteroids with long term remission after withdrawal, suggesting a benign prognosis.
Although generally thought to be a characteristic benign syndrome with good outcomes, several studies have been published linking RS3PE to various rheumatic disorders such as spondyloathropathies, psoriasis (HLA associations), polymyalgia rheumatica, and temporal arteritis. 3 It may also be a paraneoplastic manifestation of haematological or solid malignancies 4 (eg. prostate, rectal, gastric and ovarian tumors) linked to the synthesis of interleukin, IL-6. Review of these cases suggested that RS3PE associated with neoplasia was associated with a poor response to steroid treatment. 4
Although MRI scanning offers the best imaging technique to diagnose the condition.,RS3PE is a clinical diagnosis. Scans typically demonstrate the tenosynovitis of the extensor tendons believed to cause the oedema which characterises the syndrome.3 MRIscans are valuable to exclude other bony pathologies like osteomyelitis.. An alternative imaging technique for identification of extensor tenosynovitis is ultrasonography. 5
Treatment generally involves steroids, but in some cases the patient may respond to NSAIDs or gold therapy
Learning points:
RS3PE should be considered as a diagnosis when a patient presents with bilateral symmetrical pitting oedema of the hands and or feet, and is found to be seronegative.
Patients are generally very responsive to corticosteroids.
A high index of suspicion is needed to search for underlying malignancy especially in the absence of associated rheumatic disorders and poor response to corticosteroid therapy.
COMPETING INTERESTS
None Declared
AUTHOR DETAILS
DR. VIJAY JOSHI MD, Registrar, Internal Medicine, Chase Farm Hospital, UK
DR ANNA GREEN MBBS, FY1 Doctor, Chase Farm Hospital, UK
DR. JANE GRIFFIN FRCP, Consultant Rheumatologist, Chase Farm Hospital, UK
CORRESPONDENCE: DR. VIJAY JOSHI, Chase Farm Hospital, Enfield, UK
Email: vbj_@hotmail.com
References
-
McCarty DJ, ODuffy JD, Pearson L, Hunter JB. Remitting seronegative symmetrical synovitis with pitting edema. RS3PE syndrome. JAMA 1985 254(19):2763-7
-
Mehmet Sayarlioglu Remitting Seronegative Symmetrical Synovitis with Pitting Edema (RS3PE) Syndrome and Malignancy. Eur J Gen Med 2004; 1(2): 3-5.
-
Oliveri I, Salvarani C,Cantini F. Remitting distal extremity swelling with pitting edema: a distinct syndrome or a clinical feature of different inflammatory rheumatic diseases.J.Rheumatol 1997;24:249-52
-
Sibilia J, Friess S, Schaeverbeke T et al. Remitting seronegative symmetrical synovitis with pitting edema (RS3PE): a form of paraneoplastic polyarthritis? J Rheumatol 1999;26:115-20
-
Agarwal et al . Remitting seronegative symmetrical synovitis with pitting edema (RS3PE) syndrome: ultrasonography as a diagnostic tool. Clinical Rheumatology. Volume 25, Number 5/October 2005

The above article is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License.




